Author: Dhritisree *
Every possible economic activity has been halted as the Covid-19 pandemic induced lockdown extends for almost two months in India. On one hand, India is trying hard to battle against Covid-19, on the other hand, a significant proportion of population is facing starvation. We have way passed the debate on the need of lock down. Now, the central concern is to set a balance between life and livelihood. It is evident from the current rate of new Covid-19 cases in India that the economy will not restart where it exactly stopped. Even a layman can tell that we have slipped into a world recession which can be compared with the Great Depression of 1930’s if not more. Human lives have faced and will be facing number of challenges to survive during this lock down period and in the coming days of recession. But vulnerable groups like children, pregnant women, malnourished people and the people who have already experienced a higher risk of poverty will be the most affected ones. This article highlights the possible sets of adversity encountered by infants and pregnant women during this pandemic and its long-term effects.
Antenatal care (ANC), care during child birth and post-natal care are the most important amenities that a mother and a child require to endure a long healthy life in lateral years. Absence of institutional structure of these amenities may result in maternal mortality, infant mortality (perinatal and neo-natal), health complications in mother and child, low birth weight, malnourishment, wasted or stunted growth of child and so on. In India, 59 percent of women have their first ANC visit during the first trimester of pregnancy and 51 percent have four or more ANC visit (defined by WHO) in 2015-16 (NFHS-4 Report). In the last two months, many pregnant women missed their ANC several times as there is hardly any public conveyance on the road. Additionally, fear of Covid-19 infection is keeping them away from hospital visits. Only extreme cases are possible to be addressed under such circumstances. Therefore, the aforementioned percentages will be significantly low in this year which in turn increase the complication at child birth in coming months. A key means to reduce maternal and neonatal mortality is to have an institutional delivery. Previously, the percentage of institutional deliveries were extremely low in rural areas (29 percent in 2005-06, NFHS-3 Survey) than in urban areas (68 percent in 2005-06) but the distance is reduced in recent years (75 percent in rural areas as oppose to 89 percent in urban areas in 2015-16, NFHS-4 Survey). This distance might get a little higher once again since the very presence of mid-wives in rural areas may encourage an in-house delivery so that visit to health centres could be avoided during this pandemic. This escalates the chance of mortality both for mother and child. This trait will be worse for the lowest income group since till date, only 60 percent of them seek for institutional delivery as oppose to the national average (81 percent).
Immunisation
Vaccination is a crucial part of post-natal care. India’s Universal Immunisation Programme provides free vaccines against 11 life threatening diseases like Tuberculosis, Diphtheria, Pertussis (or whooping cough), Tetanus, Polio, Hepatitis B, Pneumonia and Meningitis, Measles, Rubella, Japanese Encephalitis and Rotavirus Diarrhoea. This initiative is estimated to avert millions of deaths every year. Effectively children aged between 0 to 5 years and pregnant women are the recipients of this programme. It is one of the most efficient health investment and it is accessible even for vulnerable groups or the most hard-to-reach population in hinterland. This nationwide drive has stalled due to the current lockdown, in turn endangering millions of lives. Recently, WHO estimated that over 117 million children in 37 countries may miss out on receiving life-saving measles vaccine. UNICEF has repeatedly warned the governments to step up and resume uninterrupted immunisation services. Immunisation drive in India is primarily done by Accredited Social Health Activists or ASHA workers and community health workers under the Ministry of Health and Family Welfare (MoHFW). But currently, they are closely working with the other health workers in preventing pandemic fatality.
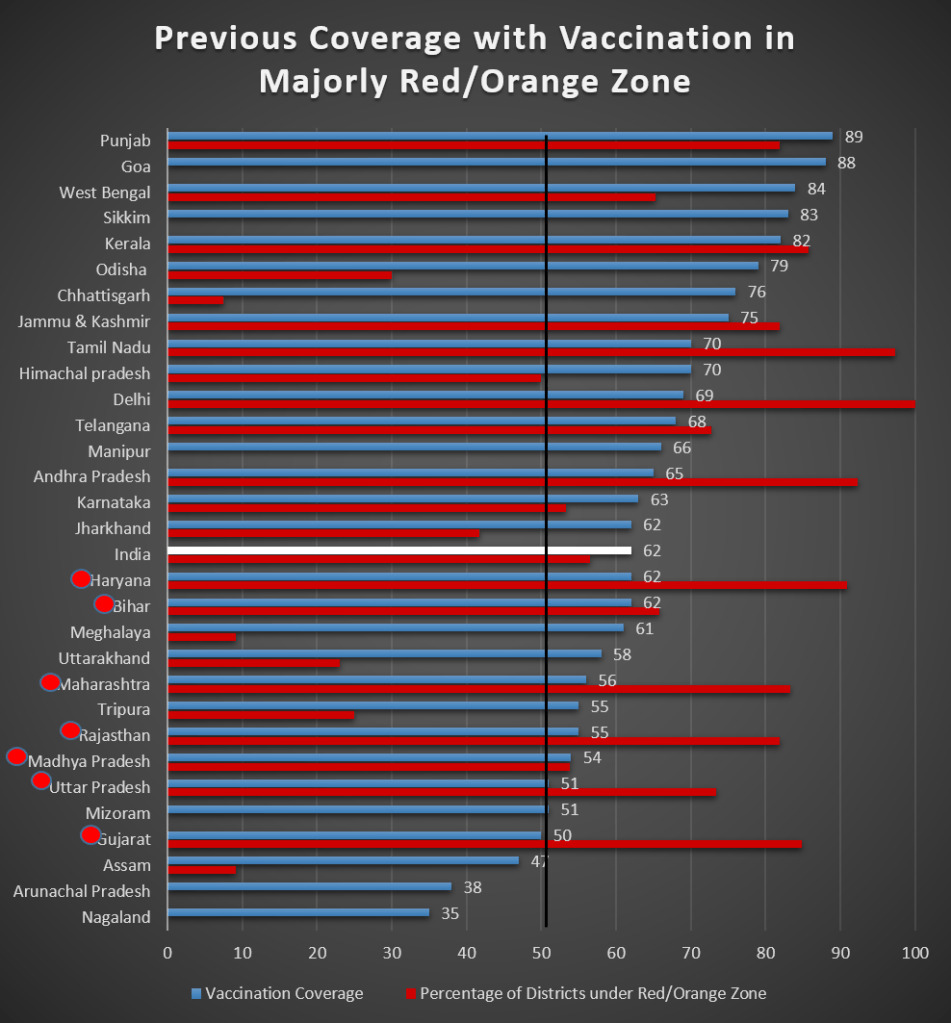
As the states are reassembling the ailing service as the nation is in the third phase of lockdown, it is the time to decide on immediate policies which are required to resolve the current crisis in terms of immunisation. According to NFHS-4 report, 62 percent of children aged 12 to 23 months received all basic vaccinations in 2015-16 (Graph Above). This vaccination coverage is not uniform across all the states. On one hand, states like Punjab, Goa, West Bengal, Sikkim and Kerala have covered almost 80 to 90 percent of children under basic vaccination, on the other hand, there are 14 states where immunisation programme could cover only the percentage of children which is less than all India average. States like Gujarat, Assam, Arunachal Pradesh and Nagaland lie at the bottom of the ladder where only 50 percent or less children have been immunised in 2015-16. Presently, all the states should resume the immunisation drive immediately but the above 14 states require special attention as they are already lagging behind in terms of coverage. Among these 14 states, there are 7 states where the percentage of districts under red or orange zone is more than 50 percent indicating higher risk of transmission of Covid-19 and limited movement in the respective states. Therefore, these states will encounter greater difficulties to cover vaccination and the situation continues to be so till these places transform into green zone. The concerned states are Haryana, Bihar, Maharashtra, Rajasthan, Madhya Pradesh, Uttar Pradesh and Gujarat. The vaccination coverage in these states happen to be comparatively low empirically even before the wide spread of Covid-19 in these states. The extensive spread will only make things worse. Hence, extra provision has to be taken in these states in coming months so that the children and pregnant women can be protected from other deadly diseases.
Malnutrition
Malnutrition among children and adults is one of the leading health concerns in India. In India, 38.4 percent children below five years are stunted, 21 percent are wasted and 35.7 percent children are underweight in 2015-16 (NFHS-4 Report). Mother’s malnutrition escalates a series of health adversity such as maternal and infant mortality, stunted or wasted growth, declined immunity, morbidity, physical and cognitive disability and therefore, poor economic outcome in adulthood. According to World Bank, 1 percent loss in adult height due to childhood stunting is associated with 1.4 percent loss in economic productivity. Anganwadi services is the largest nutrition arrangement in rural India under the scheme of Integrated Child Development (ICDS) monitored by Ministry of Women and Child Development. Anganwadi centres (AWCs) provide health, nutrition, and education services for children from birth to six years of age, as well as nutritional and health services for pregnant and breastfeeding women. Hence, these centres are primary provider of pre-natal and post-natal care in rural areas. Children receive immunisations, regular health check-up and food supplements from AWCs which are vital for their growth in the formative years. Here, received supplementary food includes both food cooked and served at an AWC on a daily basis or given in the form of take home rations. For many children in rural India, AWC is the only source of nutritious food or significant meal or worse, only meal of the day. During the initial phase of lockdown, AWCs were closed across India and only take-home rations were delivered at the door steps by the Anganwadi workers. The children belong to impoverished households are already suffering malnutrition and the additional burden of closed AWCs under lockdown takes a heavy toll on them. Almost 50 percent of the children from lower income strata availed the AWC food supplements as oppose to higher income strata (around 30 percent) in 2015-16. The halt of economic activity has forced the poor families to starvation. The only source of nutritious food for children could have been from AWCs which are either providing limited food or no food currently. Under such circumstances, malnutrition situation will be worsening in India, making moderately malnourished children to severely malnourished. The immediate policy suggestion would be to make AWCs functional at the earliest in green zone at least, especially in the states where AWCs used to be heavily beneficial.
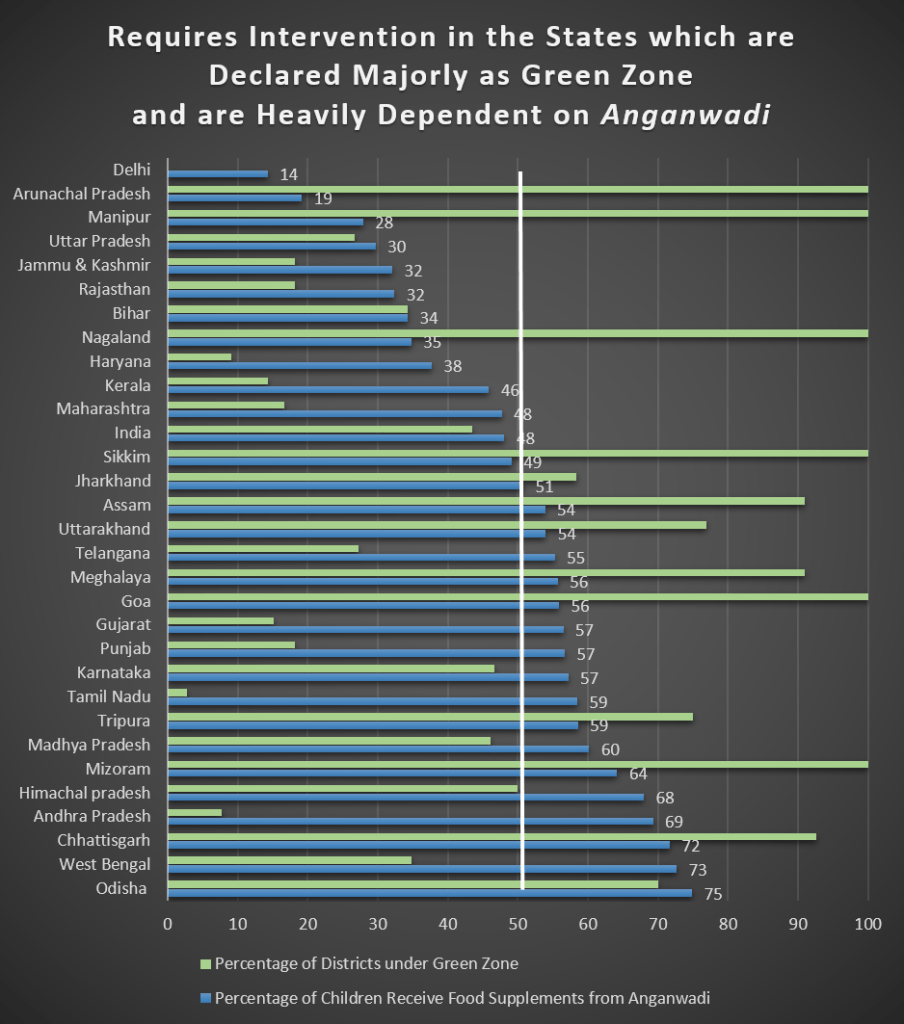
Currently, 14 states have more than 50 percent of districts under green zone (Graph Above). Out of these states, 10 states have 50 percent (or more) of children who usually receive food supplements from AWCs. Those states are Jharkhand, Assam, Uttarakhand, Meghalaya, Goa, Tripura, Mizoram, Himachal Pradesh and Chhattisgarh. These states should take initiatives to make AWCs fully operative in green zones with no shortage of food availability and should provide additional attention to the children under severe acute malnutrition (SAM) category since the need of AWCs services have mounted inexplicably, especially for low income group.
Dietary Diversity
Dietary diversity plays vital role in nutrition as it helps to achieve daily requirements of energy and other micronutrients such as vitamins, minerals to prevent morbidity. Breastfed and non-breastfed children aged 6 to 23 months are advised to get food from different food groups (i.e., minimum dietary diversity or MDD) and an optimal number of meal frequency to attain minimum acceptable diet (MAD) as prescribed by WHO. In India, 22 percent of children age 6 to 23 months meets MDD, 36 percent of them meets minimum meal frequency and only 9.6 percent of them could meet MAD in 2015-16 (NFHS-4 Report). This scarcity in MAD resulted into several morbidity conditions in children starting from Anaemia to Diarrhoea. Anaemia is a condition marked by Iron deficiency and currently, 59 percent of children aged 6 to 59 months are anaemic in India. Iodine is another essential micro-nutrient which prevents goitre or thyroid related problems. Till date, India is not a hundred percent user of iodized salt which is the essential source of iodine. Another micronutrient, Vitamin A is an essential for the immune system since severe vitamin A deficiency (VAD) can cause eye damage, leading to childhood blindness, measles and diarrhoeal disease and also, it slows recovery from illness. VAD is common in the environments where fresh fruits and vegetables are not readily available. According to NFHS-4 survey in 2015-16, around 44 percent of children aged 6 to 23 months consume foods rich in vitamin A in India. Given the last two months under lockdown, dietary diversity has become an unfeasible idea since there is a complete cease of economic activities. Both demand and supply sides are disrupted. Uninterrupted food supply is not the ground reality as promised due to temporary shutdown of multiple Mandi, conveyance shortage and limited movement in containment zones. Even demand has shrunk considerably as people are not allowed to venture out far reaching shops, number of visits to market place has reduced and more importantly, a vast section of population is left with no income. Under such conditions, dietary diversity is unattainable for many. In the scale of achieving minimum dietary diversity, the most affected states under lockdown would be the ones where restriction due to red zone will be prolonged and simultaneously, they score low in terms of dietary diversity.
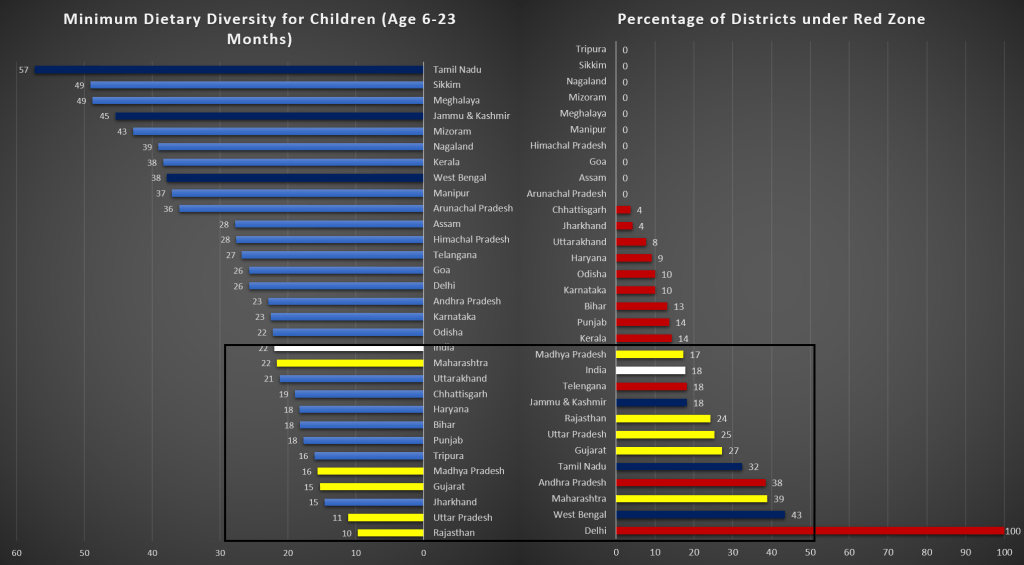
The states like Maharashtra, Madhya Pradesh, Gujarat, Uttar Pradesh and Rajasthan have only 22 percent or less children (aged between 6 to 23 months) who have achieved MDD in 2015-16 (Graph Above). These states are equally vulnerable from Covid-19 spread as the percentage of districts under red zone is 17 – 18 percent or more (say, 39 percent for Maharashtra, 100 percent for Delhi). Therefore, the children belong to these states will require extensive health support system in coming times. Another interesting reading from the graph is based on the states/UT which are at the top of the ladder considering MDD, i.e, Tamil Nadu, Jammu and Kashmir and West Bengal. The percentage of districts under red zone in these states/UT is sizeable indicating a longer inactivity in these economies. Therefore, the below mentioned higher percentages of MDD will be reduced in these places, even more so for Jammu and Kashmir as this one has undergone a long lockdown due to political turmoil previously.
Conclusion
There is no dispute on the fact that life has been disrupted world-wide. People have lost their lives and livelihood. Economy has been slowed down. The end of the tunnel is not quite visible yet. At this juncture, this article has tried to provide a partial depiction of a larger health adversity that India might face in coming days along with the other after effects of Covid-19. Among the other hitches, infants and pregnant women across the nation are confronting additional challenges. These challenges accelerate with inadequate livelihood. Therefore, pre-natal and post-natal care services, Anganwadi system, maternal health centers/hospitals and immunisation drive seek additional attention to avoid long term health hazards in the population. Mother and her children’s lives are at stake.

The painting above is a masterpiece by one of the greatest avant-garde women artists of the early 20th century, Amrita Sher-Gil. The name of the painting is ‘Mother India’. The Hungarian-Indian painter was deeply influenced by realism and was exceptionally talented in portraying the lives of people living in countryside. Her bold stroke and bright colours expressed the melancholy of their mundane life. This specific painting is a magnificent illustration of her work where a mother’s concern for her children and their impoverished living have been portrayed on the canvas. The hopelessness and anguish of their lives are marked by their large gloomy eyes. The painting is relevant like never before as the lockdown continues in India and uncertainty looms large. As every day is passing by, the mothers are getting anxious about the future of their children, uncertainty is growing for their infants and unforeseen is unfolding for the ones who are yet to be born.
Note: All the referred data related to health have been collected from NFHS-4 Survey report, 2015-16. The UTs are not considered in the graphs to improve visibility. Only Delhi and Jammu and Kashmir are considered since Delhi is the capital and Jammu and Kashmir was a state in 2015-2016. The data on Ladakh from covid19india.org is added to Jammu and Kashmir to make the data comparable.
*Dhritisree is a PhD in Economics from Indira Gandhi Institute of Development Research (IGIDR), Mumbai. She did her Masters in Economics from Jawaharlal Nehru University, New Delhi. Her research areas include Development Economics, Gender, Health and Agricultural Economics.
Kindly note that the point of views expressed in the article are entirely the author’s personal views. IPD takes no responsibility for the same.
One comment